Still, a home test is not the best fit for everyone. The right choice depends on symptoms, medical history, and what a clinician needs to measure.
What is a home sleep study in Perth?
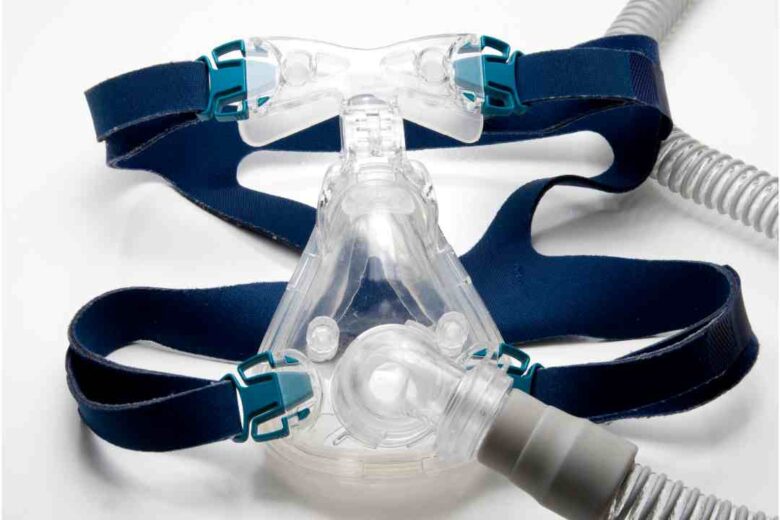
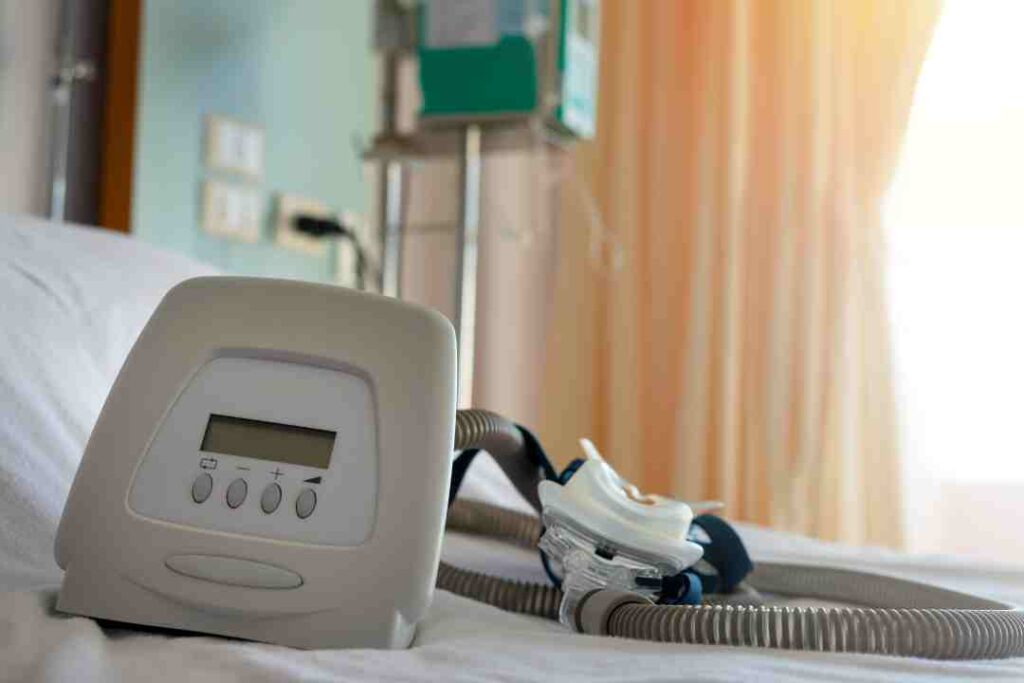
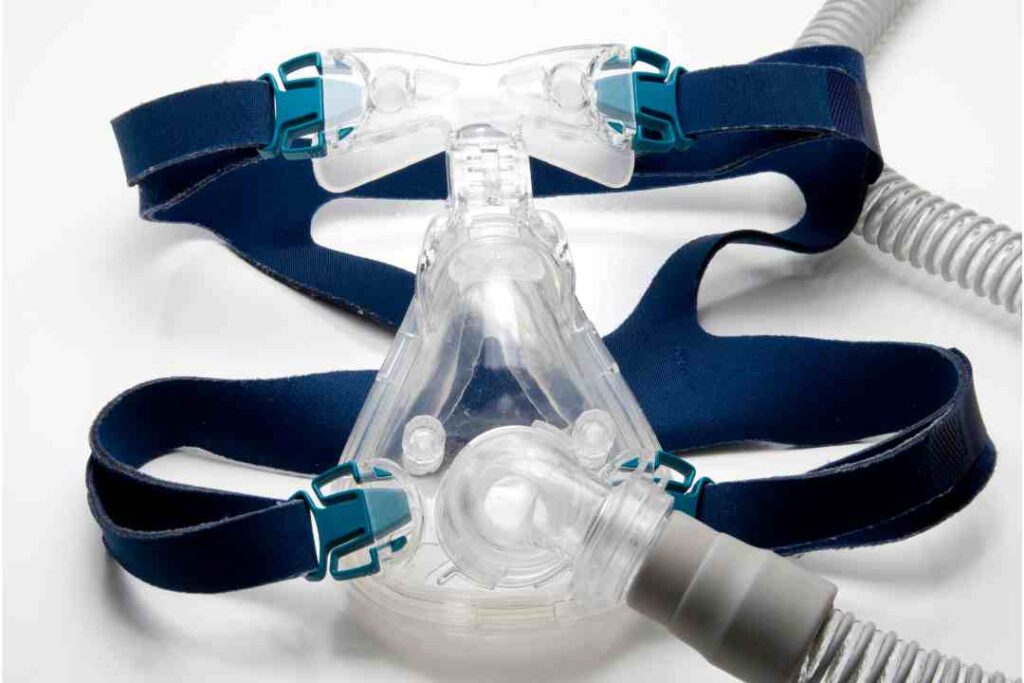
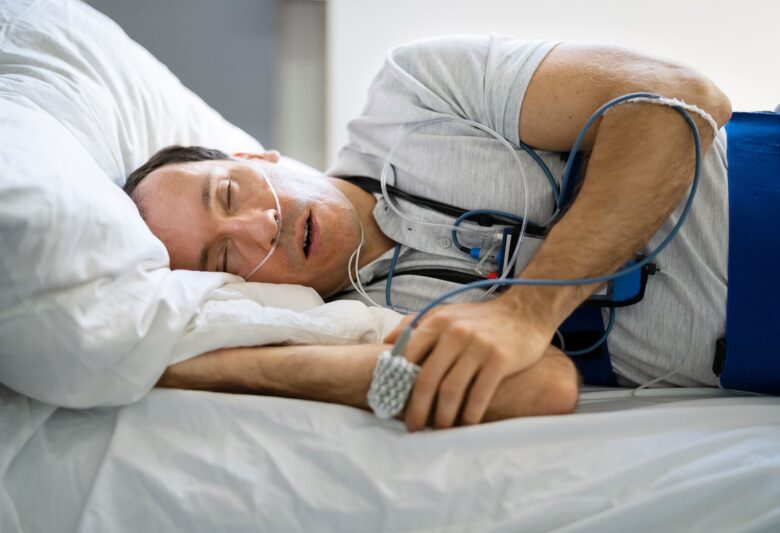
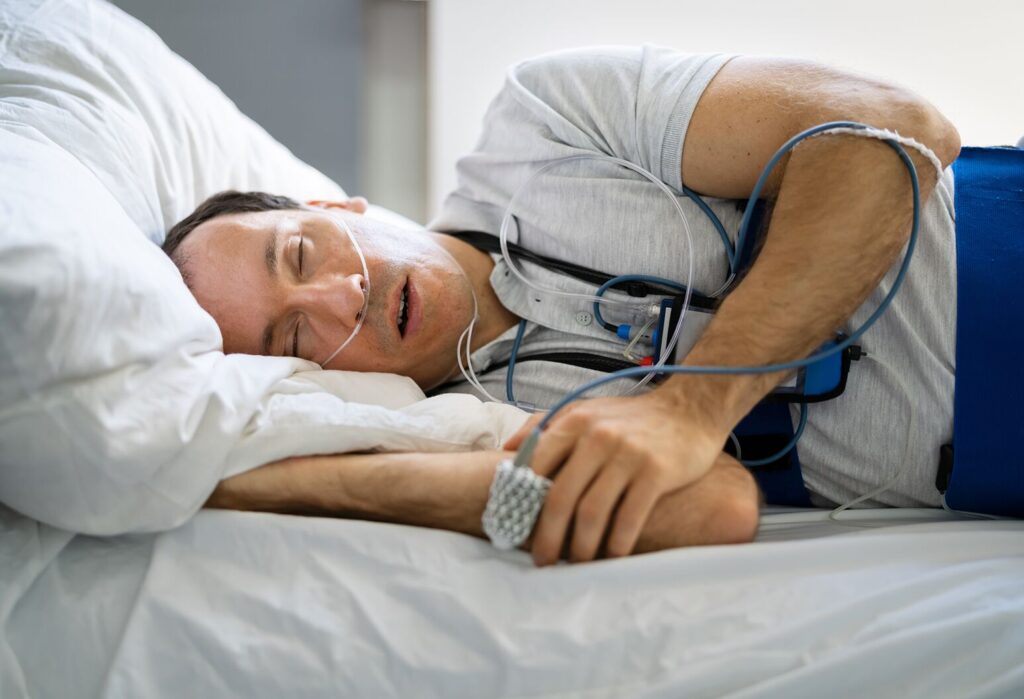
A home sleep study is a take-home test that records breathing and related signals overnight to assess for sleep-disordered breathing, most commonly obstructive sleep apnoea. During the test, the patient usually wears a small monitor with sensors placed on the finger, chest or abdomen, and near the nose.
If you’re searching for a sleep study Perth bulk billed option, it’s important to note that eligibility often depends on your referral, Medicare criteria, and the provider. In Perth, home sleep studies are typically arranged through a GP, a sleep physician, or a sleep clinic, with results interpreted by qualified professionals.
Who is a home sleep study usually right for?
A home sleep study is often suitable for people with a moderate to high likelihood of obstructive sleep apnoea. Common clues include loud habitual snoring, witnessed breathing pauses, waking with choking or gasping, and significant daytime sleepiness.
It can also suit people who prefer testing at home due to comfort, work schedules, caring responsibilities, or difficulty sleeping in unfamiliar environments.
What symptoms suggest they should consider one?
They may consider a home sleep study if they snore loudly most nights and feel unrefreshed despite adequate time in bed. Morning headaches, dry mouth on waking, irritability, poor concentration, and dozing off while reading or watching TV can also be relevant.
If partners report pauses in breathing, that is a particularly strong reason to seek assessment, even if the person feels they “sleep fine”. You may like to visit https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/sleep-deprivation to get more about sleep deprivation.
What does a home sleep study actually measure?
Most home sleep studies measure airflow, oxygen saturation, breathing effort, and heart rate, then estimate breathing interruptions such as apnoeas and hypopnoeas. Some devices also record body position and snoring.
What they usually do not measure is full sleep staging via brain waves, which is why they can be less suitable for diagnosing conditions beyond breathing-related sleep disorders.
How accurate are home sleep studies compared with lab studies?
For suspected obstructive sleep apnoea in otherwise straightforward cases, home sleep studies can be highly effective and are widely used in clinical practice. They often provide enough information to confirm the diagnosis and guide treatment.
However, they may miss or underestimate issues if sensors dislodge, if sleep time is hard to estimate, or if the suspected problem is not primarily breathing-related.
When is an in-lab sleep study a better choice?
An in-lab study may be better when there are complex symptoms or medical factors that require more comprehensive monitoring. This can include suspected central sleep apnoea, certain heart or lung conditions, neuromuscular disorders, parasomnias, seizure concerns, or unexplained insomnia.
If a clinician needs brain-wave data to analyse sleep stages, arousals, or unusual night-time behaviours, a laboratory study is usually the more appropriate test.
What is the process like from referral to results in Perth?
They typically start by speaking to a GP or sleep specialist, who reviews symptoms, risk factors, medications, and relevant health history. If a home study is appropriate, the clinic provides equipment and instructions, sometimes with a short in-person fitting or a video walkthrough.
After the night of testing, the device is returned, data is analysed, and a report is issued. A follow-up appointment usually explains the findings and outlines next steps, such as CPAP trials, lifestyle changes, or further testing.
What should they do to prepare for the night of testing?
They should follow the clinic’s instructions carefully and aim for a “normal” night that reflects typical sleep. That usually means avoiding unusual caffeine or alcohol intake, keeping their standard bedtime, and ensuring sensors are applied securely.
If they use nail varnish or acrylic nails, it can interfere with some finger oxygen sensors, so they may need to remove it beforehand. They should also tell the clinic about nasal congestion, as it can affect airflow readings.
What happens if the home study is inconclusive?
If the recording is incomplete or results do not match symptoms, a clinician may recommend repeating the home study or progressing to an in-lab assessment. Inconclusive results do not mean “nothing is wrong”; they often mean the test could not capture enough reliable data.
They should also ask whether other conditions might explain symptoms, such as restless legs syndrome, circadian rhythm issues, medication effects, anxiety, or depression.
What treatment options might follow a positive result?
If obstructive sleep apnoea is confirmed, treatment may include CPAP therapy, which keeps the airway open using gentle air pressure. Some people may be offered an oral appliance (often via a dentist with sleep training) if appropriate for their anatomy and severity.
Weight management, reducing alcohol close to bedtime, treating nasal obstruction, positional therapy, and reviewing sedating medications can also play a role. The best plan depends on severity, symptoms, and individual preferences.
How can they decide if a home sleep study is right for them?
A home sleep study is often a practical first step when symptoms strongly suggest obstructive sleep apnoea and there are no major complicating medical issues. It offers convenience, comfort, and a faster path to answers for many people in Perth.
They should choose based on clinical advice, not convenience alone. If symptoms are complex, if safety is a concern, or if initial results do not explain how they feel, they may be better served by an in-lab study or specialist review.

Related : Sleep Study Sydney Cost: Medicare and Private Pricing Explained
FAQs (Frequently Asked Questions)
What is a home sleep study in Perth and how does it work?
A home sleep study in Perth is a take-home overnight test that records breathing and related signals to assess for sleep-disordered breathing, most commonly obstructive sleep apnoea. Patients wear a small monitor with sensors on the finger, chest or abdomen, and near the nose. These studies are arranged through a GP, sleep physician, or sleep clinic, with results interpreted by qualified professionals.
Who is suitable for a home sleep study in Perth?
Home sleep studies are typically suitable for individuals with moderate to high likelihood of obstructive sleep apnoea, indicated by symptoms such as loud habitual snoring, witnessed breathing pauses, waking with choking or gasping, and significant daytime sleepiness. It also suits those who prefer testing at home due to comfort, work schedules, caring responsibilities, or difficulty sleeping in unfamiliar environments.
What symptoms suggest that someone should consider a home sleep study?
Symptoms indicating consideration of a home sleep study include loud snoring most nights, feeling unrefreshed despite adequate time in bed, morning headaches, dry mouth on waking, irritability, poor concentration, and dozing off while reading or watching TV. Notably, if partners report pauses in breathing during sleep, assessment is strongly recommended even if the person feels they “sleep fine”.
How accurate are home sleep studies compared to in-lab studies?
For suspected obstructive sleep apnoea in straightforward cases, home sleep studies can be highly effective and widely used clinically. They often provide sufficient information to confirm diagnosis and guide treatment. However, they may miss or underestimate issues if sensors dislodge or if the problem is not primarily breathing-related. In such cases, in-lab studies may be more accurate.
When is an in-lab sleep study preferred over a home sleep study?
An in-lab sleep study is preferred when there are complex symptoms or medical factors requiring comprehensive monitoring. This includes suspected central sleep apnoea, certain heart or lung conditions, neuromuscular disorders, parasomnias, seizure concerns or unexplained insomnia. In-lab studies also provide brain-wave data necessary for analysing full sleep stages and unusual night-time behaviours.
What should patients expect during the process from referral to results for a home sleep study in Perth?
Patients usually start by consulting a GP or sleep specialist who reviews their symptoms and health history. If appropriate for a home study, equipment and instructions are provided with fitting guidance. After testing overnight at home following normal routines and preparation instructions (like avoiding caffeine), the device is returned for analysis. A follow-up appointment explains findings and outlines next steps such as CPAP therapy or further testing.